Polycystic ovary syndrome (PCOS) has confounded doctors from the moment they gave the condition its name.
In people with ovaries, PCOS has historically been defined by abnormally high levels of androgens—hormones that typically regulate male sexual development—that lead to irregular menstrual periods, abnormal ovulation and often infertility, as well as other symptoms such as acne or excess facial or body hair. But over the past several decades, a better understanding of PCOS’s root causes has led to a strange connection. Many men who are related to people with PCOS seem to share many of the same symptoms that stem from what researchers think causes PCOS: a genetic susceptibility that leads to metabolic dysfunction, which in turn causes insulin resistance that disrupts hormone signaling.
This awareness has led the medical community to advocate for a name change that is more aligned with the syndrome’s root causes for the condition, STAT reported earlier this month (Slate reported on this previously). If it happens, researchers hope this change could open the doors for more treatments and better diagnosis of the condition in all those who experience it.
On supporting science journalism
If you’re enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
It Was Never about the Cysts
Back in the 1930s, physicians Irving Stein and Michael Leventhal identified a cluster of symptoms in some women that included enlarged ovaries, irregular or absent periods and infertility. To treat the condition then, doctors would cut out, or resect, a wedge-shaped portion of the ovary. For reasons that are still not fully understood, the treatment sometimes worked; many people started ovulating again.
When Stein and Leventhal looked at the resected ovarian tissue, they saw many small, fluid-filled sacs lining the edges, which to them looked like cysts. These “cysts” became the defining feature of the condition that was soon named polycystic ovary syndrome.
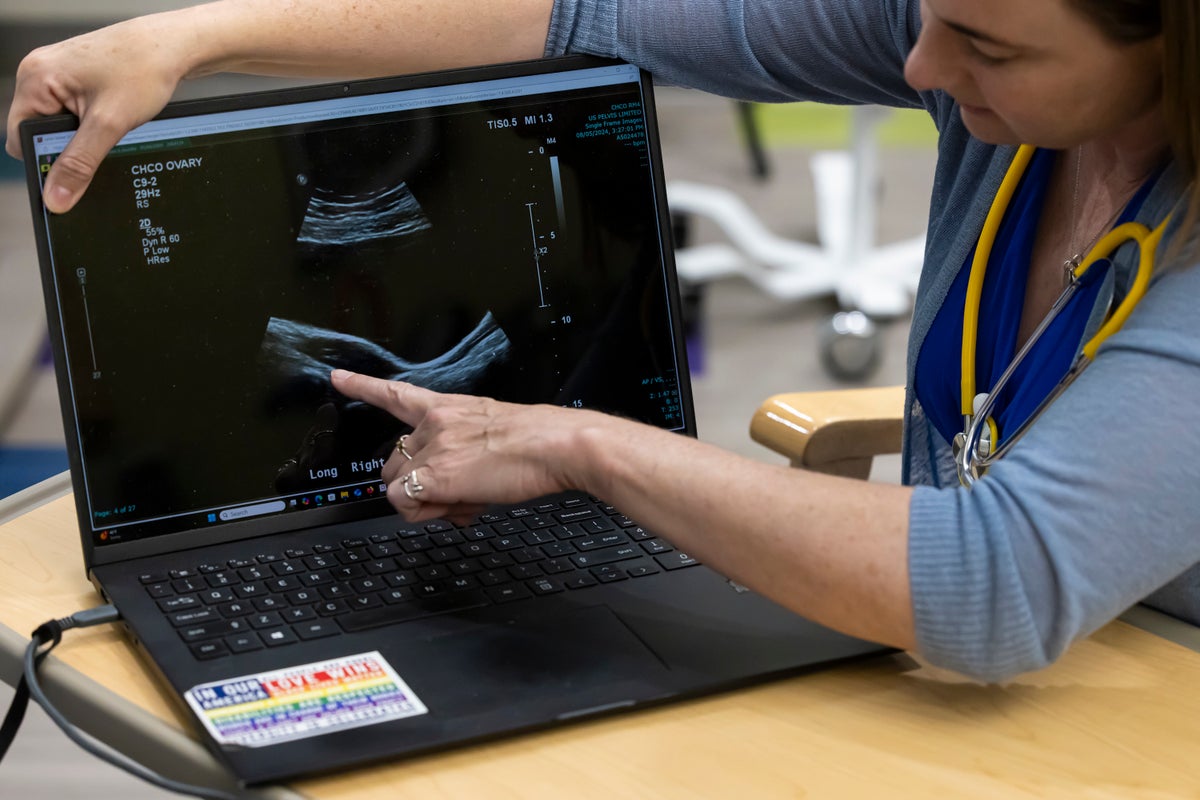
There was only one problem: because imaging technology for the condition didn’t exist at the time, those surgeons didn’t realize that they were actually looking at follicles (not cysts), which contained underdeveloped eggs that had failed to mature and release. On ultrasounds today, they resemble a string of pearls. Unlike cysts, they don’t grow or rupture.
Still, the name stuck—and with it, so did misunderstanding about the condition. Over the past several decades, however, researchers have been slowly chipping away at what drives the syndrome and who it affects.
“Polycystic ovary syndrome is the single most common hormonal disorder in women” of reproductive age, says Ricardo Azziz, a professor of reproductive endocrinology and gynecology at the University of Alabama at Birmingham, who has spent a large part of his career studying the syndrome. “It’s a global disease, and [it] affects between 10 and 15 percent of all women globally,” Azziz says.
But of those affected, he says, studies suggest only about half are properly diagnosed. PCOS seems to have both multiple causes and multiple presentations. “It is not a single disorder,” Azziz says. “It’s a collection of signs and features.”
Doctors now recognize four distinct phenotypes of PCOS, many of which don’t require the signature excess follicles. Azziz and endocrinologist Andrea Dunaif say one aspect researchers have settled on is that a person’s genetics heavily influence whether or not they develop PCOS.
In their research, Azziz and Dunaif have found that the condition clustered in families. From there, “we were able to show that if you were the sister of a woman with PCOS, you had about a 40 or 50 percent increased risk in having it, and that also led to the question, ‘Well, if it’s inherited and it’s not sex-linked [or passed on the X chromosome], which it didn’t seem to be, are men affected?’” says Dunaif, a professor of molecular medicine at the Icahn School of Medicine at Mount Sinai in New York City.
In one form of PCOS that occurs in people with ovaries, a genetic susceptibility increases the risk of insulin resistance. Insulin is a hormone produced by the pancreas that helps move sugar from the blood into other cells in the body. But if a person’s body doesn’t respond appropriately to insulin, the pancreas ends up producing even more insulin to compensate, leading to high amounts of both glucose and insulin in the blood. The high levels of insulin then stimulate the ovaries to produce excess androgens—notably, testosterone—which can disrupt normal follicle development and ovulation, leading to irregular menstrual cycles and other PCOS symptoms.
Now researchers are finding that this underlying genetic susceptibility to insulin resistance and elevated androgen levels can also show up in men.
“Almost 20 years ago we did studies where we looked at the brothers and the fathers [of women with PCOS] to see if they had any of the features of PCOS as well,” Dunaif says. “We found that the men had increased risk for being overweight, for having metabolic syndrome—and the younger men also had higher levels of a male hormone made by the adrenal glands,” she says. “This suggested that these were genetic features.”
The problem is that while men are clearly experiencing these issues, “there’s virtually no awareness among the medical community,” particularly in general internal medicine, Dunaif says. “The tragedy of PCOS has been that the specialties that ought to care about it don’t know about it.”
What’s in a name?
This new understanding of PCOS has led many experts to call for a name change—to one that is tied to the genetic and metabolic underpinnings of the syndrome instead of mistakenly focused on cysts.
Researchers from across the world have recently come to an unofficial agreement on a new name for PCOS, though it’s being kept under wraps for now. Dunaif, who knows the newly proposed name but can’t divulge it, says she’s unsure if it will even make it through the name change process. Researchers already went through this process once, in 2012, when there was a coordinated effort amongst a group of researchers and physicians to rename PCOS to “metabolic reproductive syndrome.” But this would have been abbreviated as “MRS,” which could have perpetuated the female-focused nature of the syndrome, Dunaif says.
A shift in the lexicon could increase awareness not just among physicians and patients but also in researchers studying the condition. There is precedent for this. For example, the condition now known as metabolic syndrome used to be called syndrome X—named simply because the exact mechanism wasn’t yet understood. The change helped unify research and improve diagnosis because it made the underlying mechanism clearer to both doctors and patients. Dunaif says that medical research databases show how once the name was changed, there was suddenly an explosion of research on metabolic syndrome.
Azziz agrees a name change could help the many people who have PCOS. “This is a huge population. Ten to 15 percent of all women have PCOS and perhaps 10 to 15 percent of men have PCOS, and we have not a single—not one—drug that is actually [Food and Drug Administration] approved for PCOS directly,” he says. “If more funding was available…, then we would be able to have much better treatments and targeted treatments for PCOS than we currently have.”