Several U.S. passengers onboard the cruise ship at the center of a deadly hantavirus outbreak are back in the country and under medical watch. They will quarantine for 42 days—many of them at a special facility—while they are monitored for signs of infection.
The length of sequestration is to cover the incubation period of the virus, or the time from exposure to signs of infection. But the Andes virus, the type of hantavirus involved in the outbreak, has “a much longer incubation period than we see for a lot of other viruses,” said Brendan Jackson, acting director of the Division of High-Consequence Pathogens and Pathology at the Centers for Disease Control and Prevention, at a Monday news conference. Because symptoms can take weeks to show up, additional cases could still emerge, complicating public health efforts to contact trace possible exposures and transmission chains.
Of the 18 passengers who returned this week to the U.S., at least one person has tested positive for the Andes hantavirus, which has killed three passengers who had been on the 147-person cruise that was diverted to the Canary Islands. On Tuesday the World Health Organization director announced that a total of 11 cases have been reported in the outbreak.
On supporting science journalism
If you’re enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
The passengers in the U.S. are currently being monitored at a quarantine unit in Nebraska and at a biocontainment unit in Georgia, but they will be allowed to complete the surveillance period at home if they remain asymptomatic, said Department of Health and Human Services officials at a media conference at the University of Nebraska Medical Center, where 16 of 18 the U.S. passengers are currently staying. The remaining two—a symptomatic person and their spouse who had no symptoms—were transferred to Atlanta for treatment and monitoring.
Seven passengers who had already returned to the U.S. during a planned early disembarkation on April 24 before any cases had been reported are self-monitoring at home in several states, including Arizona, California, Georgia, Texas and Virginia, under state health surveillance. HHS officials also said that risk of Andes virus to the general public is still low. But the situation is rapidly evolving and things could change.
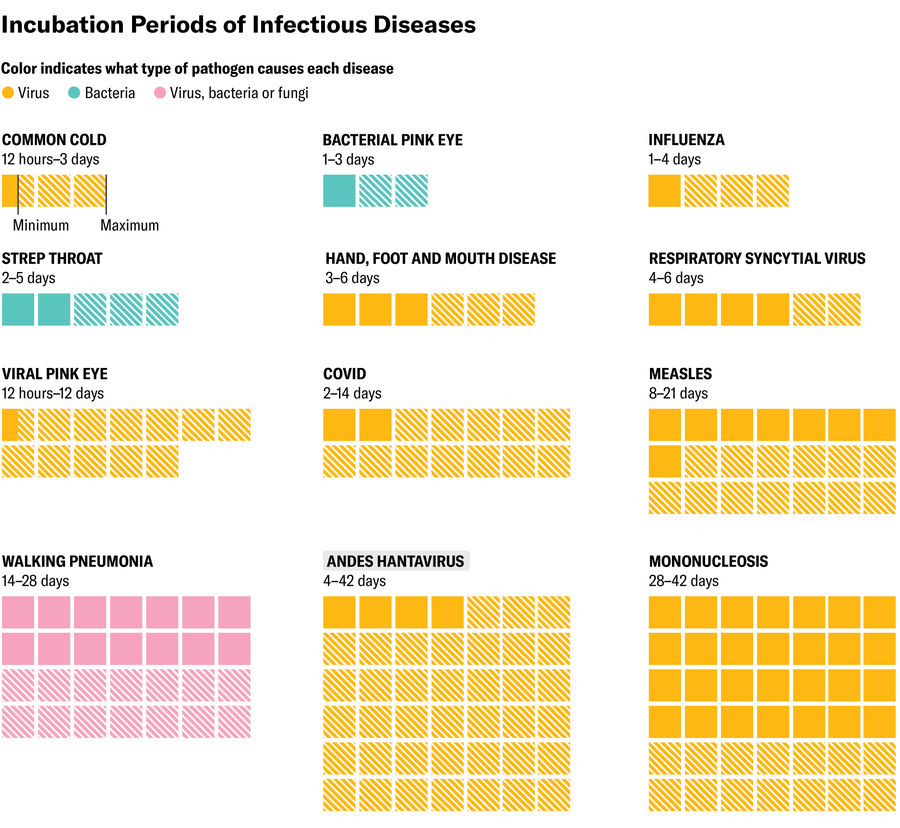
Amanda Montañez; Source: Cleveland Clinic, U.S. Centers for Disease Control and Prevention (data)
A lengthy incubation
Hantaviruses are a broad family of viruses, and different types can have varying incubation periods, says Daniel Pastula, chief of neuroinfectious diseases and global neurology at the University of Colorado Anschutz. Since the 1990s, studies on Andes virus have indicated an incubation range of four to 42 days, with most people showing symptoms around the second to fourth week after exposure, says Greg Mertz, a physician and professor emeritus of internal medicine at the University of New Mexico, who has studied hantaviruses for decades. “There’s a possibility that the incubation period could be as long as seven weeks, but that’s uncommon,” he says.
Based on the timeline of cases in the current outbreak reported to date, Pastula estimates that the incubation period has been two to three weeks, which is within the expected range. But several factors might influence the length of incubation. Although hantaviruses are primarily spread through exposure to infected rodents or their feces or urine, the Andes virus is the only hantavirus type known to spread human-to-human.
“Whether they get it through a mouse bite, inhaling aerosolized mouse excrement [or from close contact with] an infected human, I think that all probably plays a role in what the incubation periods are,” Pastula says. Those different sites of infection might influence the speed of disease progression. The viral load is also a factor—the bigger the dose of virus particles the body is exposed to, the sooner people get sick, he says.
The Andes virus’s comparatively long incubation time could also reflect how it attacks the body and initially evades immune detection. Other respiratory viruses such as influenza (which typically incubates for between one and four days) or the COVID-causing virus SARS-CoV-2 (which has a two to 14-day incubation period, depending on the variant) rapidly replicate in the upper airways, where they can infect and transmit between people quickly.
“You can tell from influenza that local infection starts in the upper respiratory tract,” Mertz says. That’s less clear with Andes virus, which can cause “widespread infection without developing an immune response [at first].”
Research shows the Andes virus can quietly circulate in the bloodstream from the initial site of infection. Eventually it infiltrates endothelial cells lining blood vessels throughout the body but primarily in the lungs. The virus replicates there without immediately killing cells and triggering an immune response. Over time, infection and delayed immune activity cause inflammation and fluid to build up in the lungs, making it hard to breathe.
Researchers believe the disease is likely most transmissible when people become symptomatic, but it’s not clear when the infectious period begins and how long it lasts after a person has recovered, Pastula says. Studies have shown that the virus can be present in the blood and other bodily fluids weeks before symptoms start. In a 2007 study in Chile, researchers took blood samples of 76 people infected with Andes virus and 476 household contacts. “Since we were following these household contacts prospectively, we were able to collect blood samples weekly for several weeks before they became symptomatic,” says Mertz, who co-authored the study. “We were able to detect virus in blood for up to 14 days before the patients became symptomatic.”
Another study of people hospitalized with Andes virus infections, published last year in the Lancet Infectious Diseases, also found the virus in blood, as well as in saliva and another fluid in the mouth, even in the final stage of infection. It is not yet clear whether Andes hantavirus can be transmitted before people show symptoms, however, Pastula says. And while infection can be confirmed through polymerase chain reaction (PCR) testing, a positive result doesn’t tell clinicians whether someone is currently infectious, he says.
Longer incubation periods can reduce pathogens’ ability to spread quickly from person to person, which typically gives public health officials the upper hand in identifying contacts and monitoring them to control outbreaks. But it can complicate other containment processes.
“We have such quick ability to travel around the world. I can get literally to the other side of the world in two days, and with incubation periods lasting longer than that, it’s hard to potentially do that contact tracing” to warn others who may have been exposed, Pastula says. “This requires not only a whole robust public health surveillance and response locally, but it requires coordination between different public health entities.”