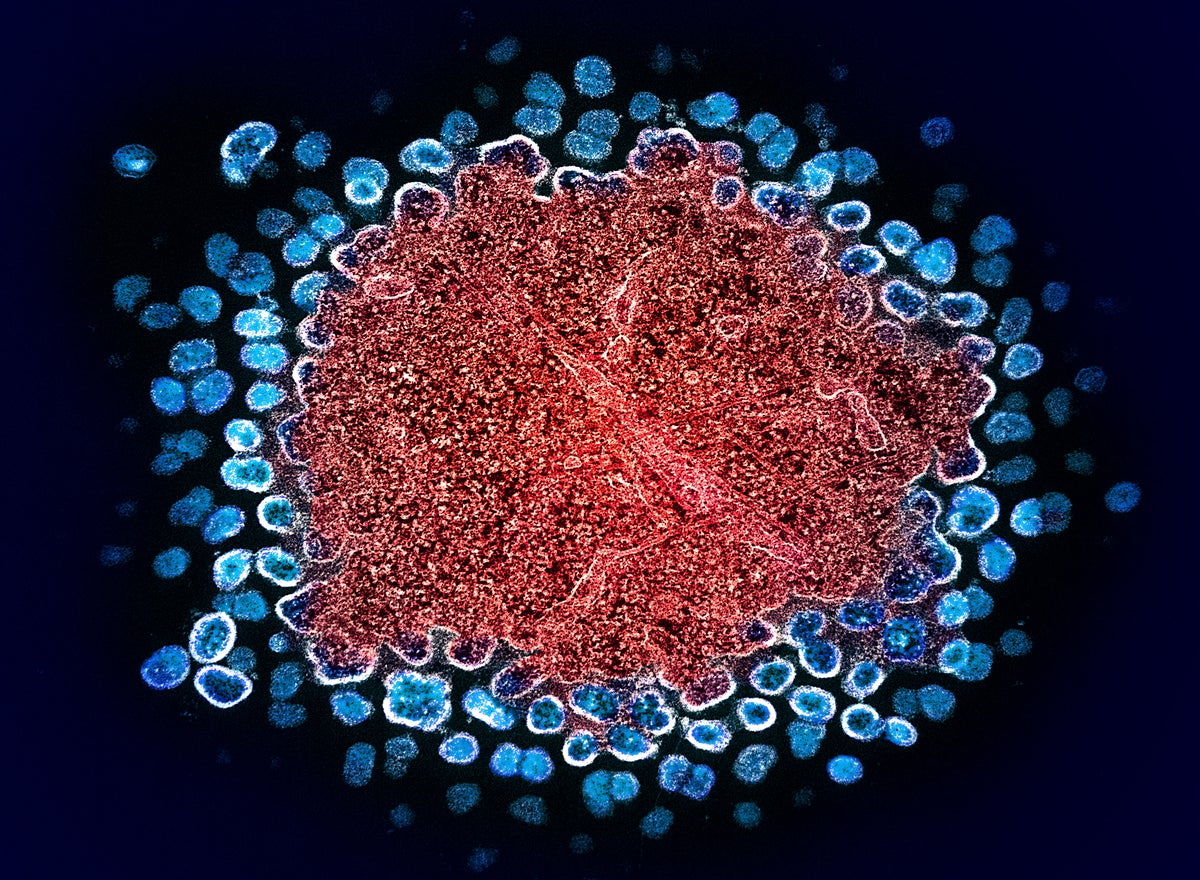
Person functionally cured of HIV after bone marrow transplant from sibling
A man with HIV has gone into remission after receiving bone marrow from his brother, who has a rare mutation that prevents the function of receptors that HIV binds to
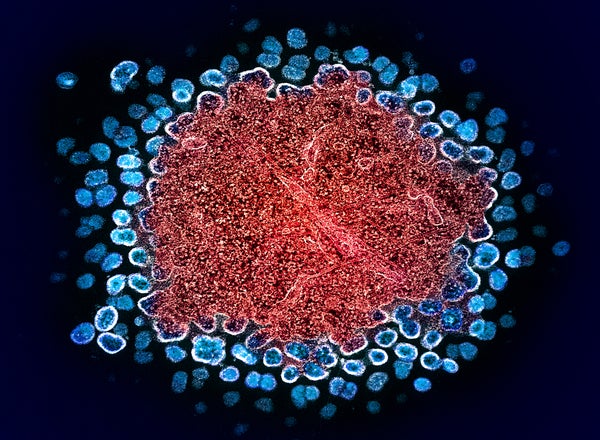
Colorized transmission electron micrograph of numerous HIV-1 virus particles (blue) replicating from a segment of a chronically infected H9 T cell (red).
A 63-year-old man has been functionally cured of HIV with a bone marrow transplant. While bone marrow donations have resulted in HIV remission in the past, this is the first time that has occurred with a donation from the recipient’s sibling.
The man received a bone marrow donation from his brother, who has a rare genetic mutation called CCR5Δ32 that confers resistance to HIV-1, the most common type of human immunodeficiency virus. When a person has two copies of this genetic mutation, the CCR5 surface protein, to which HIV commonly binds, is prevented from being expressed on human immune cells called T cells. A paper published today in Nature Microbiology showed how, after the transplant, the donor cells had replaced the HIV-positive man’s bone marrow cells and their genes had two copies of a CCR5Δ32 mutation (not all cells in the recipient’s body got replaced, however). His healthy T cell count soared in the year after the procedure and stayed at healthy levels after he stopped antiretroviral therapy (ART)—the gold standard treatment for HIV—two years later.
ART drugs can prevent HIV from reproducing in the body and spreading to other people. But they don’t eliminate the virus entirely—it sticks around in dormant reservoirs around the body. If a person with HIV stops taking ART, the virus begins spreading again.
On supporting science journalism
If you’re enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
In the new study, the researchers tested the recipient’s blood, gut tissues and bone marrow to search for reservoirs of HIV after the bone marrow transplant. They found no detectable HIV in the places it would normally linger in someone who was on ART.
“If this reaction does not happen in all or at least most of the immunological tissues, there might be a risk for rebound at some point,” says Marius Trøseid, an infectious disease specialist at Oslo University Hospital and a co-author of the paper. “I think we have shown, for the first time, that it’s a complete engraftment—both in peripheral blood, which has been shown in several other cases, in bone marrow, which has also been shown in a couple of other cases, and then also the gut mucosal tissue, which we think is key for [a] cure.”
But this treatment isn’t yet available for most people with HIV. Patients in New York City, London, Dusseldorf and other places who achieved HIV remission after a bone marrow transplant from a donor with a CCR5Δ32 mutation each needed it for another reason, such as cancer treatment.
“This is really only for a patient with additional malignancies or medical conditions that require a transplant because [by] itself, it’s just too risky” compared with ongoing ART treatment, says Jingmei Hsu, an oncologist at NYU Langone Health’s Laura and Isaac Perlmutter Cancer Center and lead author of the study on a patient in New York City, who was not part of the new paper.
For recipients, bone marrow transplants present significant risks, including severe infections, graft versus host disease (GVHD), in which donor cells attack the patient’s body, or even death. So “the risk of transplant needs to be substantially lower than the risk of the patient dying from their malignancy,” Trøseid says.
Through various studies that have measured the effect of a bone marrow transplant on a person’s HIV status, scientists have seen the infection go into remission even when the donor does not have two copies of the CCR5Δ32 mutation. Because the new study used donor cells from the patient’s sibling, it adds novel information about how these transplants work.
If the cells are too different from those of the donor, transplant complications such as GVHD could be more of a concern, says Björn-Erik Ole Jensen, head of the infectious disease department at the University Hospital of Dusseldorf, who was not involved in this study. If the donor cells are too similar to those of the recipient, however, there’s a risk that the treatment could fail to effectively destroy infected T cells.
“[A sibling transplant] may be a difference, but we don’t understand everything perfectly,” Jensen says. “This is why all these cases are still interesting.”
It’s Time to Stand Up for Science
If you enjoyed this article, I’d like to ask for your support. Scientific American has served as an advocate for science and industry for 180 years, and right now may be the most critical moment in that two-century history.
I’ve been a Scientific American subscriber since I was 12 years old, and it helped shape the way I look at the world. SciAm always educates and delights me, and inspires a sense of awe for our vast, beautiful universe. I hope it does that for you, too.
If you subscribe to Scientific American, you help ensure that our coverage is centered on meaningful research and discovery; that we have the resources to report on the decisions that threaten labs across the U.S.; and that we support both budding and working scientists at a time when the value of science itself too often goes unrecognized.
In return, you get essential news, captivating podcasts, brilliant infographics, can’t-miss newsletters, must-watch videos, challenging games, and the science world’s best writing and reporting. You can even gift someone a subscription.
There has never been a more important time for us to stand up and show why science matters. I hope you’ll support us in that mission.